BRCA1/BRCA2 genes, genetic testing, and modern prevention strategies.
The discovery of the BRCA1 and BRCA2 genes (1994-1995) was a significant milestone for the prevention and treatment of breast and ovarian cancer.
Since then, technological progress, reduced testing costs, and the "Angelina Jolie Effect" (2013) have led to a worldwide increase in genetic testing.
Both genes participate in DNA repair. Pathological mutations lead to reduced function and accumulation of genetic damage that ultimately causes cancer. Mutations can be inherited from either parent — each child of a carrier has a 50% chance of inheriting the mutation.
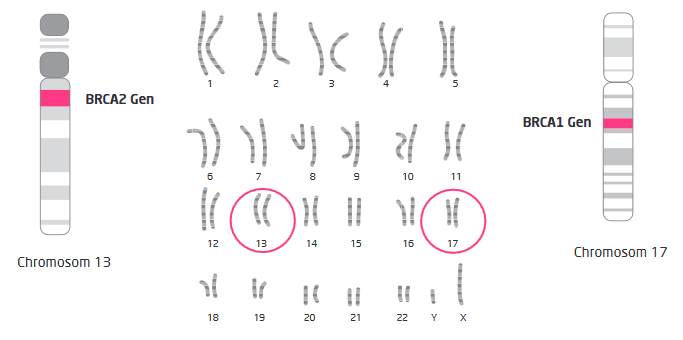
BRCA1 mutations: 50-65% risk of breast cancer and 40-65% risk of ovarian cancer by age 70. BRCA2 mutations: 40-55% risk of breast cancer and 15-25% risk of ovarian cancer by age 70. By comparison, the general population risk for ovarian cancer is only 1-2%.
According to the German Cancer Research Center, testing is recommended when: three female relatives have developed breast cancer, or one developed cancer before age 36, or one developed bilateral cancer, or there is a combination of breast and ovarian cancer in the family, or a patient with triple-negative breast cancer before age 50. Genetic counseling is essential before and after testing.
The most effective options: prophylactic bilateral mastectomy (significantly reduces breast cancer risk) and prophylactic oophorectomy after family completion (reduces ovarian cancer risk by >90%). Alternatively: intensive monitoring with annual breast MRI and mammography, transvaginal ultrasound and CA-125, as well as chemoprevention with tamoxifen or raloxifene.

At our center, we provide individualized genetic counseling and guidance for every patient. Early diagnosis and proper prevention save lives.